To better respond to rising overdose-related hospitalizations in the ByWard Market, addiction program advocates say shelters and social services should be more spread out across the city.
In Rideau-Vanier Ward alone, Action Sandy Hill estimates there are between 12 and 14 shelters, many of which provide addiction treatment among other social services.
Katie Price, the head of the substance use support program for Operation Come Home, said the location of these services often can be a trigger for people trying to manage substance use through professional help.
“I can’t tell you the number of people I’ve spoken with who are trying to get out of the lifestyle but feel like they’re continuously pulled back,” said Price.
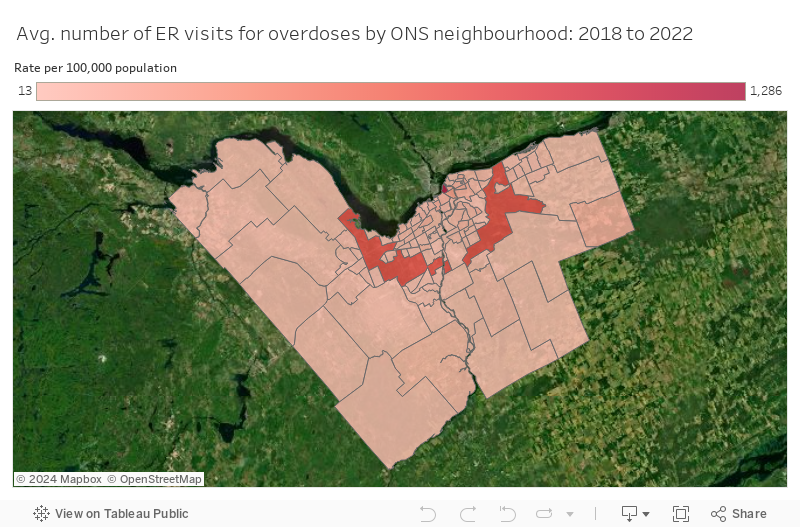
With a population of roughly 4,000 people, the ByWard Market has had an annual average of 88 emergency department visits because of overdoses between 2018 and 2022. That’s the equivalent of 1,285.9 per 100,000 people, according to data supplied by the City of Ottawa.
This rate is nearly 10 times higher than all other neighbourhoods. Sandy Hill and Vanier South, both in Rideau-Vanier Ward alongside the Market, also appear in the top five for overdose emergency department visits.
With the concentration of overdoses in her ward stretching back decades, Rideau-Vanier Counc. Stéphanie Plante said she attributes the abundance of these addiction and homelessness services to past discriminatory practices in the city.


“[O]ver the years, people who have these kinds of setbacks have congregated in this area,” the councillor said. “Because we’ve clustered all of these people in one area, it actually leads to worse outcomes.”
Rob Boyd, the CEO of Ottawa Inner City Health, agrees.
“I think that there’s very likely a correlation in terms of the much higher levels of poverty in these wards,” he said.
Many neighbourhoods within Rideau-Vanier possess lower-than-average income rates than most city neighbourhoods, according to the Neighbourhood Equity Index.
Helping to improve the community
People experiencing lower levels of income and education are often more likely to experience opioid poisoning-related hospitalizations.
In a written statement to Capital Current, the Amethyst Women’s Addiction Centre said that factors related to people’s social instability have played a critical role in these increased visits due to overdoses.
“We believe that people’s social context contributes to why people turn to substance use, so as economic and housing insecurity increase, so too does the need for coping and substance use is often people’s attempt at finding psychological and emotional relief,” said Amethyst Women’s Addiction Centre.
“Nobody chooses to struggle with addiction … if people understood that it was just someone’s way of trying to cope with something really damaging, that may change perceptions a little bit.”
Katie Price, substance use support program head for Operation Come Home
While many maintain that clustering these services in Rideau-Vanier is the biggest factor limiting their effectiveness, these services are still essential to providing vital care to those living with substance use disorders.
OICH, in conjunction with Shepherds of Good Hope, operates a consumption site known as The Trailer near the ByWard Market.
It is one of three consumption sites within Rideau-Vanier, with the other two operated by the City of Ottawa and the Sandy Hill Community Health Centre.
These sites allows use of narcotics under the supervision of health professionals.
Health Canada says the supervision provided helps alleviate the risk of accidental overdoses and often reduces the number of overdose-related emergency department visits.
OICH also runs an emergency department diversion program, allowing those who have an overdose outside of their consumption site to have a bed within a shelter that has the same level of support supervision as a hospital emergency department.
OICH and Shepherds are also involved in a pilot study of a new safer supply program.
Since 2017, fentanyl began to dominate the Ottawa drug supply, said Boyd. Fentanyl is far more potent than other opiates such as heroin, even a small amount could be lethal.
The emergence of fentanyl is part of the troubling evolution of an unregulated drug market.
“The nature of the unregulated supply is that it keeps changing, new things keep getting introduced, and we have zero control over that,” said Boyd.
And, with the variable nature of this unregulated drug market, Boyd said people cannot always determine what they are purchasing and the dosages can range.
A safer supply program, Boyd said, works to lower these risks for people who are frequently overdosing by providing them with prescription opioids with hopes of lowering dependence on an unregulated drug market.
“Some people have completely stopped using the unregulated market; some people continue to use the unregulated market along with their safer supply,” Boyd said. “We’ve even had a few cases of people who’ve completely stopped using substances.”
As of September, among other initiatives, Ottawa Public Health has pledged to post the results of the city’s safer supply programs online.
In late October, the city also announced the creation of an emergency shelter crisis task force with hopes of relieving the stress on existing shelters. Along with Mayor Mark Sutcliffe, Plante was one of many councillors who signed on to the task force.
Is this enough?
Many advocates still argue that these city programs are small steps in truly reducing rising overdose rates.
Following the COVID-19 pandemic, heightened loneliness and anxiety have drastically increased substance use across a broad spectrum of people.
“Loneliness was a big, big stressor for a lot of folks, especially folks that were living with chronic houselessness,” said Kim Hellemans, a Carleton University neuroscientist. “We were told ‘don’t be around other people.’ So what were they doing? They were using alone. What does that put you at risk for? Using alone and overdosing.”
Hellemans says the pandemic has created a crisis among at-risk populations, which continues to put pressure on a strained healthcare system as the complexity of healthcare issues increases.
As the community-based social service network for addiction and mental healthcare erodes, Amethyst said folks need to wait longer and longer for inadequate service, potentially increasing their risk of continuing to use unsafe supply in unsafe conditions.
Local organizations providing addiction and consumption services have tried to respond, but many have been overwhelmed and it has become increasingly hard to communicate with substance-using communities in the aftermath of COVID-19.
“There is a community amongst people who use drugs, and that became very fragmented and destroyed during [the pandemic],” said Boyd. “So, we’re beginning to start working more with the community to rebuild the leadership and to rebuild some of those community norms that existed prior to COVID.”
Those norms include re-establishing a “looking out for each other approach” and assessing how many in the community can best integrate within the larger community in the neighbourhood, said Boyd.
A recent trend of substance users smoking rather than injecting their drugs has also continued to increase the strain on resources said Boyd, even though Ontario consumption sites are smoke-free.
“We are now responding to more opiate overdoses outside of our sites than we are inside,” Boyd said. “And this is because of people smoking.”
In October, Ottawa Public Health updated its Overdose Response Strategy, which aims to expand access to health and substance-use services across the city. Notably, it recommends that the chair of the Board of Health request, among other things, that the Ontario Ministry of Health provide funding for safer inhalation services and expand drug checking services.
Referring to the report, Plante said she does not support its definition of community as solely substance-users. She feels it fails to recognize the experiences of others in her ward affected by substance use.
With five fatalities a week in her ward and the feeling they are always behind the ‘innovation of those who are trying to sell drugs,’ Plante said she fears what impact the next opioid entering the community will have, especially for youth.
“I always really, really worry about the kids because I don’t think you should grow up walking to school fearful of seeing syringes or finding syringes in your school yard,” said Plante.
Looking ahead
Other than increasing the capacity for the safer supply pilot program, which only has a capacity of 500 people, Boyd said Ottawa could better address the overdose crisis by first developing and running permanent housing with additional health care and support for people reliant on drugs.
In particular, Boyd cited a growing number of substance users in need of 24-hour support, as multiple overdoses can lead to brain injuries.
“Certainly, we want people to live as independently as possible. But with brain injury, for a lot of folks, that’s not really going to be an option for them to be able to maintain independent living,” said Boyd. “And so they’re going to need that extra level of support that’s offered through supportive housing.”
The second important factor is to increase funding and support for drug-checking services and provide safer spaces for those who are going to continue to use illicit drugs, Boyd said.
When investing in these services specifically to address the overdose crisis, Amythest said they must be fully funded by the healthcare system and provide a continuum of care.
“We need commitment from the City of Ottawa and the provincial government to provide dedicated, stable funding of harm reduction services to address the overdose crisis,” said Amythest.
Most importantly, Price said that allowing services to spread across the city would do more than relieve stress on ByWard Market. It would provide aid to people suffering in other parts of Ottawa.
As highlighted by Amethyst, healthcare in Canada is a universal right, and it should be granted to everyone without conditions, even those with substance use disorders.
“I think we’re all responsible at some level to do what we can, and that doesn’t mean donating money and this kind of thing, because not everyone can do that,” said Price. “But just even bringing awareness, talking about these things, kind of taking away from the stigma.”
If Ottawa residents wish to learn more about substance use, they can head to capsa.ca.